Purchased Care Alternative Analysis – Evaluation of Business Strategic Options
by Logapps LLC
June 25, 2015

Logapps Delivered an Analysis of Alternatives for a Claims Processing System to Support the Department of Veterans Affairs.
Introduction
The Purchased Care Program Office of the Veterans Health Administration’s (VHA) Chief Business Office contracted with Logapps through TCA to provide an independent Analysis of Alternatives in four parts: claims processing, Health Administration Center (HAC) Eligibility System, Fee Authorization Module, and Program Level Approach. This paper represents the completion of the first of those four tasks the review of alternatives for the replacement of the current claims processing system.
Challenge
The U.S. Department of Veterans Affairs (VA) utilizes the Purchased Care Programs to pay for healthcare services provided to veterans and eligible dependents from non-VA healthcare providers. The VA manages the processing of claims through approximately 150 VA Medical Centers (VAMCs) across the United States. Claims processing for the Fee Program has long been outdated and inefficient. As a result, there are often over payments, duplicate payments, and erroneous payments that total tens of millions of dollars annually.
Approach
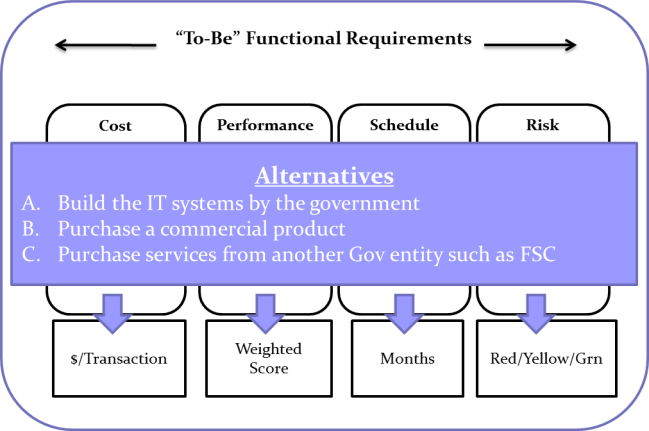
The VA provided three alternatives for the Team to analyze and recommend the best solution for a replacement claims processing system. They were:
A. Build the information technology (IT) systems by the government: CBO Purchased Care custom development solution via VA’s Office of Information and Technology (OI&T), with management and claims processing operations located in Denver, CO.
B. Purchase a commercial product: CBO Purchased Care commercial-off-the-shelf (COTS) purchase and modification solution, via the VA’s Office of Information and Technology (OI&T), with management and claims processing operations located in Denver, CO.
C. Purchase services from another Government entity, such as the VA’s Financial Services Center (FSC): FSC COTS solution. Operations located in Denver, CO, and Austin, TX.
Additionally, at the time of the study, non-VA healthcare claims were processed at approximately 150 separate sites, which increased the opportunity for erroneous payments and increased the operational costs of the program. Therefore, Logapps studied centralization of operations in each of the three alternatives.
Logapps used an analysis model that measured each alternative by four operational parameters: Schedule, Cost, Performance, and Risk. Schedule determined the amount of time it would take to develop and fully deploy the alternative. The Cost category measured both the development and operational costs over aten-year period, with the results provided in then-year dollars. Performance measured the degree to which an alternative met the operational needs of the VA and was expressed as a percentage of satisfied requirements. Risk measured the probability and severity of undesirable events and was depicted against red/yellow/green risk cubes.
A significant amount of research was conducted for the analysis of alternatives. Artifacts were collected and interviews were also conducted. Specifically, the efforts associated with the analysis encompassed the review of over 1,500 pages of documentation collected from HAC, FSC, and commercial vendors; review of over 90 documents obtained through open literature research; seven information gathering trips to five cities in which Logapps conducted in-person interviews and contacted roughly 125 individuals; and two stakeholder workshops for Risk and Performance.
Interested in learning more? Please contact us today.